Kleienpilzflechte
Begutachtet von Dr Doug McKechnie, MRCGPZuletzt aktualisiert von Dr Philippa Vincent, MRCGPZuletzt aktualisiert 26. Feb 2025
Erfüllt die Anforderungen des Patienten Richtlinien des Patienten
- HerunterladenHerunterladen
- Teilen
- Language
- Diskussion
- Audio-Version
Medizinische Fachkräfte
Fachartikel sind für die Nutzung durch Gesundheitsfachkräfte konzipiert. Sie werden von britischen Ärzten verfasst und basieren auf Forschungsergebnissen, britischen und europäischen Richtlinien. Möglicherweise finden Sie einen unserer Gesundheitsartikel nützlicher.
In diesem Artikel:
Lesen Sie unten weiter
What is pityriasis versicolor?
Pityriasis versicolor is a common skin complaint in which mildly scaly, discoloured patches appear mainly on the chest and back. It is sometimes called tinea versicolor, although it is not actually a tinea as this strictly refers to infection with a dermatophyte fungus.
It is caused by the proliferation of the lipophilic fungus of the genus Malassezia (früher bekannt als Pityrosporum) which is part of the normal flora of human skin.
Usually Malassezia spp. grow sparsely in the seborrhoeic areas (scalp, face and chest) without causing a rash. However the fungus may change from its normal form to a pathological mycelial form.
Pathogenic forms may be triggered by various factors, including humidity and high temperature, hyperhidrosis, familial susceptibility, and immunosuppression. The most common Malassezia species associated with pityriasis versicolor is M. globosa, with M. sympodialis und M. furfur also frequently seen.1
How common is pityriasis versicolor? (Epidemiology)2
Zurück zum InhaltIt occurs worldwide but is most common in hot and humid climates. It occurs more often in the summer than in the winter months in temperate zones.
Prevalence may be up to 50% in some tropical countries compared with less than 1% in temperate climates.3
It most often affects teenagers and young adults. It is less common in infants and the elderly.
It occurs in people of all skin types but the changes in pigment are more obvious in those with darker skin.3
Most infections occur in normal healthy people but the following factors increase the risk:
Hyperhidrosis or increased physical activity causing sweating.
Occlusive clothes, dressings or ointments.
Immunosuppression or immune deficiency.
Malnutrition.
Lesen Sie unten weiter
Symptoms of pityriasis versicolor
Zurück zum InhaltIt usually has an insidious onset and in some cases it can be several months before it is noticed. People often present following a holiday where they have become more tanned and therefore the paler discoloured areas are more apparent.
Macular lesions and patches of altered pigmentation are seen primarily on the trunk.
These lesions frequently spread to the neck, upper arms and abdomen and can sometimes occur at other sites. The rash is usually seen in sebum-rich sites. The face may be affected in some.
There is a superficial scale which is best seen by stretching the affected skin, or scraping the surface.
Pityriasis versicolor close-up
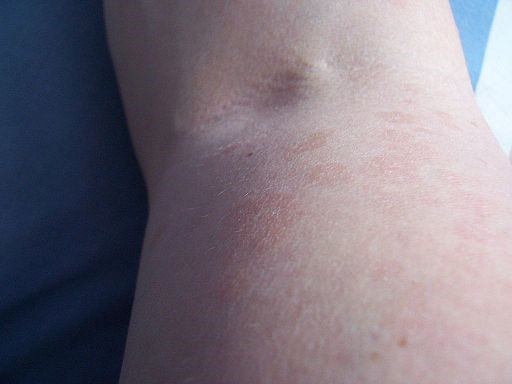
© Richardkiwi at nl.wikipedia (Own work), Public domain, via Wikimedia Commons
Pityriasis versicolor on the forehead
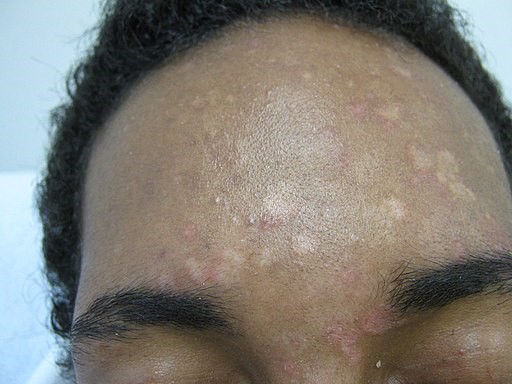
© Grook Da Oger (Own work) CC BY-SA 3.0, via Wikimedia Commons
Sometimes the patches start scaly and brown and then resolve through a non-scaly and white stage.
Itching, if present, is mild.
Pityriasis versicolor is not contagious, as it is a commensal yeast.
Differentialdiagnose
Zurück zum InhaltPityriasis alba.
Seborrhoische Dermatitis (may co-exist).
Secondary Syphilis.
Lesen Sie unten weiter
Untersuchungen
Zurück zum InhaltInvestigations are not usually necessary, as the diagnosis is often made clinically. They may be necessary if the condition is not responding to treatment or if the diagnosis is unclear. Where required, skin scrapings can be sent for microscopy. The spores and hyphae have a 'spaghetti and meatball' appearance on potassium hydroxide wet-mount examination. Yellow to yellow-green fluorescence may be observed on examination of affected areas with a Wood's light. There is no benefit of fungal culture, as the organism is part of the normal flora and isolation is therefore not necessarily relevant.
Treatment for pityriasis versicolor234
Zurück zum InhaltPityriasis versicolor should be treated initially with topical antifungals, especially topical imidazoles - eg, clotrimazole, miconazole, econazole and ketoconazole in various formulations (creams or shampoos).
Ketoconazole shampoo is usually first-line and should be applied on to affected areas and made into a lather; it should then be left for five to fifteen minutes before washing off. This should be repeated daily for a week and then weekly for a month.56
Selenium shampoo can be used as an alternative although unlicensed for this indication. It should be diluted with water (to reduce the likelihood of irritation), applied to affected areas for ten minutes and then rinsed off. This should be repeated daily for seven to ten days. This is contra-indicated in pregnancy.
If very small areas are involved, or in pregnancy, antifungal imidazole creams such as clotrimazole may be used as an alternative. The cream should be applied twice a day for two to three weeks.
In widespread or resistant cases, prescribe itraconazole 200 mg daily for seven days (although terbinafine is active against dermatophytes (eg, tinea), it actually has little effect on yeast infections). Alternatively, fluconazole may be used - 50 mg daily for two to four weeks, or 300-400 mg weekly for one to three weeks.
Oral treatments should be avoided with a history of heart failure or liver failure. There is a risk of acute liver failure with use of oral antifungal treatments. 7Oral treatments should not be used if pregnant or breastfeeding.
Patients should be advised that it can take several months for the skin colour to return to normal.
Antifungal treatment should be repeated when the scaly component of pityriasis versicolor recurs.
Recurrences of pityriasis versicolor are common.
Prophylaxe
For those who are prone to develop recurrent episodes in warm or humid environments, they can be advised to use ketoconazole shampoo prophylactically once a day for three days prior to any exposure.
Ketoconazole or selenium sulfide shampoo may be applied for five to ten minutes one to four times monthly for those who have frequent recurrences.
Komplikationen
Zurück zum InhaltInfection often leads to hypopigmentation of the skin, which may persist for months after successful treatment.
Prognose
Zurück zum InhaltPink or brown types of pityriasis versicolor generally clear satisfactorily with treatment but the rash often recurs.
The pale type of pityriasis versicolor also generally clears up with treatment and the skin eventually responds normally to sun exposure.
White marks are occasionally permanent and resistant to antifungal treatment.
Weiterführende Lektüre und Referenzen
- Pityriasis Versicolor; DermIS (Dermatologisches Informationssystem)
- Kleienpilzflechte; DermNet NZ
- Gupta AK, Foley KA; Antifungal Treatment for Pityriasis Versicolor. J Fungi (Basel). 2015 Mar 12;1(1):13-29. doi: 10.3390/jof1010013.
- Kleienpilzflechte; NICE CKS, Oktober 2023 (nur für UK-Zugang)
- Leung AK, Barankin B, Lam JM, et al; Tinea versicolor: an updated review. Drugs Context. 2022 Nov 14;11:2022-9-2. doi: 10.7573/dic.2022-9-2. eCollection 2022.
- Renati S, Cukras A, Bigby M; Pityriasis versicolor. BMJ. 2015 Apr 7;350:h1394. doi: 10.1136/bmj.h1394.
- Britisches Nationales Arzneimittelverzeichnis (BNF); NICE Evidenzdienste (nur in Großbritannien zugänglich)
- Pityriasis Versicolor; Dermnet
- https://bnf.nice.org.uk/drugs/itraconazole/
Lesen Sie unten weiter
Artikelverlauf
Die Informationen auf dieser Seite wurden von qualifizierten Klinikern verfasst und begutachtet.
Nächste Überprüfung fällig: 25. Feb 2028
26. Feb 2025 | Neueste Version

Fragen, teilen, verbinden.
Durchsuchen Sie Diskussionen, stellen Sie Fragen und teilen Sie Erfahrungen zu Hunderten von Gesundheitsthemen.

Fühlen Sie sich unwohl?
Bewerten Sie Ihre Symptome online kostenlos