Vorhofflimmern und Schlaganfallprävention
Begutachtet von Dr Hayley Willacy, FRCGP Zuletzt aktualisiert von Dr Colin Tidy, MRCGPLast updated 19. Dez 2024
Erfüllt die Anforderungen des Patienten Richtlinien des Patienten
- HerunterladenHerunterladen
- Teilen
- Language
- Diskussion
- Audio-Version
In dieser Serie:Vorhofflimmern
Die Medikamente, die zur Vorbeugung eines durch Vorhofflimmern bedingten Schlaganfalls eingesetzt werden, heißen Antikoagulantien. Diese helfen, die Bildung von Blutgerinnseln in Ihren Blutgefäßen zu verhindern.

Unsicher beim Mischen von Medikamenten?
Überprüfen Sie mögliche Wechselwirkungen zwischen Medikamenten, Nahrungsergänzungsmitteln und Lebensmitteln, bevor Sie sie zusammen einnehmen.
In diesem Artikel:
Video picks for Herz- und Blutmedikamente
Lesen Sie unten weiter
Why does atrial fibrillation increase your risk of having a stroke?
The main complication of Vorhofflimmern (AF) ist ein increased risk of having a stroke. AF can interfere with the blood flow in the heart chambers. This sometimes leads to a small blood clot forming in a heart chamber.
A clot can travel in the blood vessels until it becomes stuck in a smaller blood vessel in the brain (or sometimes in another part of the body). Part of the blood supply to the brain may then be cut off, which causes a stroke. Strokes due to AF tend to be even more serious than strokes due to other causes.
The risk of developing a blood clot and having a stroke varies, depending on several factors. The level of risk can be calculated by your doctor using a set of specific questions. This will help to decide what treatments are required. All people except those at the lowest risk will be offered medication to help prevent clots from forming.
How can the risk of stroke be reduced?
Zurück zum InhaltMedicines called anticoagulants can be used to reduce the risk of a blood clot and so reduce the risk of stroke. Anticoagulants work by prolonging the time it takes for blood to form a clot. Some people call anticoagulation 'thinning the blood', although the blood is not actually made any thinner.
Anticoagulants reduce the risk of stroke by nearly two thirds. In other words, these treatments can prevent about 6 out of 10 strokes that would have occurred in people with AF.
Lesen Sie unten weiter
Should you take medicine to reduce your risk of stroke?
Zurück zum InhaltYour doctor can use a risk assessment to see if you should take medicine to reduce your risk of stroke. The most commonly used risk assessment tool is called the CHA2DS2-VASc risk score. Points are added for each of the following it they apply to you:
Congestive heart failure with a recent exacerbation (1 point).
Hypertension - past or present (1 point).
Aged 75 years or older (2 points).
Diabetes (1 point).
Past history of a Stroke oder transitorische ischämische Attacke (2 points).
Vascular disease - for example, periphere arterielle Verschlusskrankheit, Angina or previous Herzinfarkt (1 point).
Age 65-74 years (1 point).
Sex category (ie female sex scores 1 point and male scores 0).
The higher the total points score, the higher the risk of stroke. Everyone with a score of 2 or more should be treated with anticoagulation. Men with a risk of 1 may be offered anticoagulation. Women with a risk of 1 (in other words, where female sex is their only risk factor) are not offered anticoagulation because the benefits of treatment are likely to be outweighed by the risks.
Another risk score called the HAS-BLED score is used to estimate the risk of major bleeding when you are taking a medicine to reduce the risk of stroke if you have AF. This helps to decide whether or not steps should be taken to reduce your risk of bleeding if you take anticoagulation.
A risk score called ORBIT can be used to assess your risk of major bleeding, including bleeding into the brain. For most people, the benefit of anticoagulation outweighs the bleeding risk. However, if your bleeding risk is high and cannot be reduced, your doctor will discuss the pros and cons of starting (or stopping) anticoagulation.
The National Institute for Health and Care Excellence (NICE) advises that the ORBIT risk score should be used instead of HAS-BLED to assess the risk of major bleeding when starting blood-thinning medication and whilst you are on it. This is because the evidence shows that it has a higher accuracy in predicting the risk of bleeding than other bleeding risk tools.
The CHA2DS2-VASc stroke risk score and ORBIT bleeding risk score should be reassessed at least annually.
Which medicines help to reduce the risk of stroke?
Zurück zum InhaltAspirin is very effective at reducing the risk of a second stroke if you have had a stroke which was not due to AF. However, where AF-related stroke is concerned, aspirin is much less effective than other treatments but just as likely to cause problems. It is therefore no longer recommended to reduce the risk of stroke in AF.
Instead, your doctor is likely to recommend an anticoagulant. In the past, Warfarin was the traditional option. However, several newer agents called direct-acting oral anticoagulants (DOACs) are now available. These are called:
Studies have shown the DOACs to be at least as effective as warfarin for reducing the risk of an AF-related stroke. In addition, they:
Carry a lower risk of bleeding into the brain.
Need much less frequent blood monitoring (you do not need regular INR blood clotting tests).
Have fewer interactions with other medications or food. These interactions could otherwise result in you being more prone to bleeding or clotting.
Do not require you to adjust the dose frequently dependent on your blood results, as warfarin does.
As a result, NICE has updated its guidance to recommend that DOACs should be offered in preference to warfarin. If you are already taking warfarin, your doctor may discuss changing you to treatment with a DOAC, depending on the results of your blood tests.
To find out more about these medicines, including the risks and benefits of the various alternatives, see the separate leaflet called Anticoagulants.
Lesen Sie unten weiter
Operation
Zurück zum InhaltAn operation can be used to reduce the risk of stroke for people with AF. The operation is called left atrial appendage occlusion and closes a pouch in the heart, called the left atrial appendage.
NICE in the UK has recommended that left atrial appendage occlusion can be considered as a treatment option to reduce the risk of stroke in people with AF. However, it does carry risks. It is therefore reserved for people who are at high risk of stroke and who cannot take anticoagulants.
Patient picks for Herz- und Blutmedikamente

Behandlung und Medikamente
Periphere Vasodilatatoren
Periphere Vasodilatatoren sind Medikamente, die zur Behandlung von Erkrankungen eingesetzt werden, die die Blutgefäße in den äußeren (peripheren) Teilen des Körpers betreffen, wie z.B. Arme und Beine. Zum Beispiel werden sie zur Behandlung der peripheren arteriellen Verschlusskrankheit und des Raynaud-Syndroms verwendet. Sie lindern die Symptome dieser Erkrankungen, indem sie die Blutgefäße erweitern und so verhindern, dass sie enger werden (Verengung). Diese Medikamente werden in der Regel nur verschrieben, nachdem Selbsthilfemaßnahmen ausprobiert wurden und die Symptome sich nicht bessern.
von Dr. Surangi Mendis, MRCGP
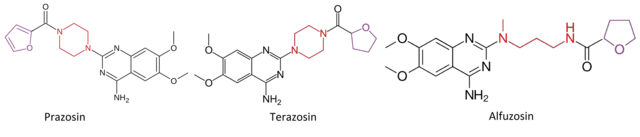
Behandlung und Medikamente
Alpha-Blocker
Alpha-Blocker sind Medikamente, die hauptsächlich zur Behandlung von Bluthochdruck (Hypertonie) und Problemen beim Wasserlassen bei Männern mit vergrößerter Prostata eingesetzt werden. Die Vergrößerung der Prostata wird auch als gutartige Prostatahyperplasie (BPH) bezeichnet.
von Dr. Doug McKechnie, MRCGP

Unsicher beim Mischen von Medikamenten?
Überprüfen Sie mögliche Wechselwirkungen zwischen Medikamenten, Nahrungsergänzungsmitteln und Lebensmitteln, bevor Sie sie zusammen einnehmen.
Weiterführende Literatur und Referenzen
- Vorhofflimmern: Diagnose und Behandlung; NICE-Richtlinie (April 2021 - zuletzt aktualisiert Juni 2021)
- Vorhofflimmern; NICE CKS, Oktober 2024 (nur für UK-Zugang)
- Thoracoscopic exclusion of the left atrial appendage in atrial fibrillation (with or without other cardiac surgery) for the prevention of thromboembolism, NICE Interventional Procedure Guideline, June 2011
- WatchBP Home A for opportunistically detecting atrial fibrillation during diagnosis and monitoring of hypertension; NICE Medical Technologies Guidance, January 2013
- Europäische Gesellschaft für Kardiologie; Richtlinien für das Management von Vorhofflimmern, 2020
- Isaew A, Adderley NJ, Ryan R, et al; The treatment of paroxysmal atrial fibrillation in UK primary care. Heart. 2017 Jun 1. pii: heartjnl-2016-310927. doi: 10.1136/heartjnl-2016-310927.
Lesen Sie unten weiter
Artikelverlauf
Die Informationen auf dieser Seite wurden von qualifizierten Klinikern verfasst und begutachtet.
Nächste Überprüfung fällig: 18. Dez. 2027
19. Dez 2024 | Neueste Version

Fragen, teilen, verbinden.
Durchsuchen Sie Diskussionen, stellen Sie Fragen und teilen Sie Erfahrungen zu Hunderten von Gesundheitsthemen.

Fühlen Sie sich unwohl?
Bewerten Sie Ihre Symptome online kostenlos
Abonnieren Sie den Patienten-Newsletter
Ihre wöchentliche Dosis klarer, vertrauenswürdiger Gesundheitsberatung - geschrieben, um Ihnen zu helfen, sich informiert, selbstbewusst und in Kontrolle zu fühlen.
By subscribing you accept our Datenschutzrichtlinie. Sie können sich jederzeit abmelden. Wir verkaufen Ihre Daten niemals.