Anämie
Begutachtet von Dr Toni Hazell, MRCGPZuletzt aktualisiert von Dr Hayley Willacy, FRCGP Zuletzt aktualisiert 13. Feb. 2023
Erfüllt die Anforderungen des Patienten Richtlinien des Patienten
- HerunterladenHerunterladen
- Teilen
- Language
- Diskussion
- Audio-Version
In dieser Serie:Ernährungspläne für Menschen mit AnämieFolsäuremangelEisenmangelanämieMakrozytose und makrozytäre AnämieVitamin-B12-Mangel und perniziöse Anämie
Anämie bedeutet, dass Sie weniger rote Blutkörperchen als normal haben oder dass Sie weniger Hämoglobin als normal in jedem roten Blutkörperchen haben. In beiden Fällen wird eine verringerte Menge an Sauerstoff im Blutkreislauf transportiert.
In diesem Artikel:
Videoauswahl für Anämie
Lesen Sie unten weiter
Anaemia types and causes
Eisenmangelanämie
Lack of iron is the most common type of anaemia in the UK. This is called iron-deficiency anaemia. If you eat a normal balanced diet, it usually contains enough iron.
Siehe das separate Informationsblatt mit dem Titel Diäten für Menschen mit Anämie.
See also the separate leaflet called Iron-deficiency Anaemia.
Vitamin deficiency anaemia
Lack of certain vitamins such as folic acid and vitamin B12 can cause anaemia.
Siehe die separaten Broschüren mit dem Titel Folic Acid Deficiency Anaemia und Vitamin B12 Deficiency and Pernicious Anaemia.
Hämolytische Anämie
Normally, red blood cells live for about 120 days before they are broken down by the body. In haemolytic anaemia they live for a much shorter time. The anaemia occurs because your bone marrow cannot produce enough new red blood cells to replace the ones that are being broken down too quickly.
There are several reasons that this happens. Genetic conditions where there is an abnormality in the red cell membrane such as hereditäre Sphärozytose, or elliptocytosis. Conditions where there are haemoglobin abnormalities such as sickle cell anaemia oder thalassaemia - these are discussed below. And problems with the chemicals (or enzymes) that help the blood cell do its job, such as G6PD deficiency and pyruvate kinase deficiency.
Another set of conditions may arise from your immune system attacking your own red blood cells, such as autoimmune haemolytic anaemia, blood transfusion reactions and other autoimmune conditions such as systemischer Lupus erythematodes.
Some medications may cause haemolysis, such as penicillin. You can also have haemolysis caused by mechanical heart valves, Malaria and liver disease. There is a wide variety of reasons you might develop haemolytic anaemia.
Thalassämie
Thalassämie is an inherited condition affecting the blood. There are different types, which vary from a mild condition with no symptoms, to a serious or life-threatening condition. For the more severe forms of thalassaemia, modern treatment gives a good outlook, but lifelong monitoring and treatment are needed. Good treatment is important to prevent complications developing.
Sickle cell anaemia
Sichelzellenanämie (SCD) is a serious, inherited condition affecting the blood and various organs in the body. It affects the red blood cells, causing episodes of 'sickling', which produce episodes of pain and other symptoms. In between episodes of sickling, people with SCD are normally well. Long-term complications can occur. Good treatment, started early in life, can prevent complications. So, early diagnosis and specialist treatment are advised for SCD. Sickle cell trait is not the same as sickle cell disease.
Aplastische Anämie
Aplastic anaemia is a group of disorders that cause bone marrow failure. Most often no cause is found but there are also some inherited bone marrow failure syndromes. Sometimes a trigger can cause aplastic anaemia, and examples of those include drugs, viruses and toxins.
Anämie bei chronischen Erkrankungen
Some long-term illnesses may lead to anaemia. These include chronische Nierenerkrankung, Tuberkulose, chronic heart failure and malnutrition. We don't fully understand why the anaemia happens but it may be partly due to reduced production of new red blood cells. Sometimes the anaemia is mild and doesn't need treatment but there are several treatment options available as well as treating the underlying disease.
Risk factors for anaemia
Zurück zum InhaltSome conditions that cause anaemia are inherited, so having a close family member who has that condition will increase your risk.
Some medications may have an effect on the bone marrow, or on red blood cells, and cause anaemia.
The following are some situations that may have a risk of developing a lack of iron and result in iron-deficiency anaemia:
Pregnancy or childhood growth spurts. These are times when you need more iron than usual. The amount of iron that you eat during these times may not be enough.
Heavy menstrual periods. The amount of iron that you eat may not be enough to replace the amount that you lose from starken Perioden.
Poor absorption of iron. This may occur with some gut (intestinal) diseases that mean the gut is not as effective at absorbing iron - for example, coeliac disease und Morbus Crohn.
Bleeding from the gut (intestines). Some conditions of the gut can bleed enough to cause anaemia. You may not be aware of losing blood this way. The bleeding may be slow or intermittent and you can pass blood out with your stools (faeces) without noticing.
If you eat a poor or restricted diet. Your diet may not contain enough iron.
If you have a chronic condition, such as heart failure or kidney disease, you are also at risk.
Lesen Sie unten weiter
Anaemia symptoms
Zurück zum InhaltCommon symptoms of anaemia are due to the reduced amount of oxygen being carried in the body.
These include tiredness, having little energy (lethargy), feeling faint and developing shortness of breath.
Less common symptoms include headaches, a 'thumping heart' (Herzklopfen), altered taste, and ringing in the ears (tinnitus).
You may look pale. You may develop sore areas at the corners of your mouth.
You may have spoon-shaped nails, a sore tongue or hair loss.
Some people may have difficulty swallowing, hair loss oder Restless-Legs-Syndrom.
Various other symptoms may develop, depending on the underlying cause of the anaemia.
Anaemia diagnosis
Zurück zum InhaltA simple blood test can measure the amount of haemoglobin in your blood and count the number of red blood cells per millilitre (ml). Although this test can confirm that you are anaemic, it does not identify the cause of your anaemia.
Sometimes the underlying cause is obvious. For example, pregnant women and women who have heavy menstrual periods may commonly develop iron-deficient anaemia.. In these situations, no further tests may be needed and treatment with iron supplements may be advised. However, the cause of the anaemia may not be clear and so further tests may be advised.
Some causes of anaemia are more serious than others and it is important to find the reason for anaemia.
Lesen Sie unten weiter
Anaemia treatment
Zurück zum InhaltThe treatment of anaemia depends on the underlying cause. For people with iron-deficiency anaemia this may simply be iron tablets. People who do not respond well to medication may be offered a blood transfusion if they are having severe symptoms.
Those with B12 deficiency will need vitamin B12 injections. The injections are usually given frequently at the start of treatment. This quickly builds up the body's store of vitamin B12. Vitamin B12 is stored in the liver. Once a store of vitamin B12 has built up, this can supply the body's needs for several months. An injection is then only usually needed every two to three months to top up the supply.
Folic acid deficiency is treated with tablets in addition to a folate-rich diet. The tablets can be stopped if your diet improves. You may need to continue with treatment if a poor diet was not the cause of folic acid deficiency.
Currently there is no cure for sickle cell disease (SCD) other than a stem cell transplant, so lifelong treatment and monitoring are needed. There are a number of different treatments which help to prevent sickling episodes, or prevent related problems such as infection. Sometimes you might need a blood transfusion. For others it may be a course of vitamins or other more complex treatments.
Anaemia of chronic disease cannot be treated by supplements or tablets. Treatments that stimulate the bone marrow to produce more red blood cells are needed.
Anaemia outlook
Zurück zum InhaltFor the most common types of anaemia, (iron deficiency, B12 or folic acid deficiency) there are relatively simple treatments and these should keep you well. For the more complex types of anaemia (sickle cell, thalassaemia, aplastic anaemia) treatment is more complex. For example, sickle cell disease may shorten life. Without treatment, people with SCD may die in childhood, from problems such as infection. Good treatment makes a great difference. Improvements in treatment mean that life expectancy has increased. However, even with modern treatment, SCD can still cause serious or life-threatening problems.
The outlook associated with the anaemia of chronic disease, is more about the severity of the underlying condition.
Patientenempfehlungen für Anämie

Allergien, Blut und Immunsystem
Makrozytose und makrozytäre Anämie
Macrocytosis refers to red blood cells which are larger than normal. It does not cause any symptoms in itself.
von Dr. Philippa Vincent, MRCGP
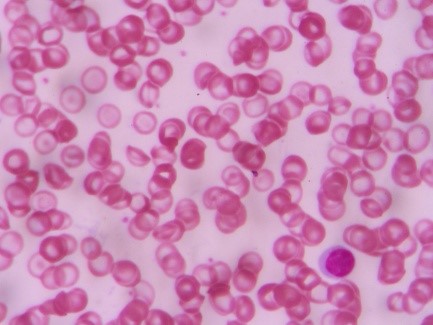
Allergien, Blut und Immunsystem
Sichelzellenanämie
Sickle cell disease (SCD) is a serious, inherited condition affecting the blood and various organs in the body. It affects the red blood cells, causing episodes of 'sickling', which produce episodes of pain and other symptoms. In between episodes of sickling, people with SCD are normally well. Long-term complications can occur. Good treatment, started early in life, can prevent complications. So, early diagnosis and specialist treatment are advised for SCD. Sickle cell trait is not the same as sickle cell disease.
von Dr. Hayley Willacy, FRCGP
Weiterführende Lektüre und Referenzen
- UK Thalassaemia Society
- Sickle Cell Society
- Anämie - Eisenmangel; NICE CKS, August 2024 (nur für UK-Zugang)
- Newhall DA, Oliver R, Lugthart S; Anaemia: A disease or symptom. Neth J Med. 2020 Apr;78(3):104-110.
- Palmer D, Seviar D; How to approach haemolysis: Haemolytic anaemia for the general physician. Clin Med (Lond). 2022 May;22(3):210-213. doi: 10.7861/clinmed.2022-0142.
- Madu AJ, Ughasoro MD; Anaemia of Chronic Disease: An In-Depth Review. Med Princ Pract. 2017;26(1):1-9. doi: 10.1159/000452104. Epub 2016 Sep 28.
Lesen Sie unten weiter
Artikelverlauf
Die Informationen auf dieser Seite wurden von qualifizierten Klinikern verfasst und begutachtet.
Nächste Überprüfung fällig: 12. Feb. 2028
13. Feb. 2023 | Neueste Version

Fragen, teilen, verbinden.
Durchsuchen Sie Diskussionen, stellen Sie Fragen und teilen Sie Erfahrungen zu Hunderten von Gesundheitsthemen.

Fühlen Sie sich unwohl?
Bewerten Sie Ihre Symptome online kostenlos
Abonnieren Sie den Patienten-Newsletter
Ihre wöchentliche Dosis klarer, vertrauenswürdiger Gesundheitsberatung - geschrieben, um Ihnen zu helfen, sich informiert, selbstbewusst und in Kontrolle zu fühlen.
Mit dem Abonnieren akzeptieren Sie unsere Datenschutzrichtlinie. Sie können sich jederzeit abmelden. Wir verkaufen Ihre Daten niemals.