Verletzungen der Kniebänder
Begutachtet von Dr Hayley Willacy, FRCGP Zuletzt aktualisiert von Dr Colin Tidy, MRCGPZuletzt aktualisiert 10. Feb 2023
Erfüllt die Anforderungen des Patienten Richtlinien des Patienten
- HerunterladenHerunterladen
- Teilen
- Language
- Diskussion
- Audio-Version
In dieser Serie:SportverletzungenOberschenkelverletzungLeistenzerrungKnöchelverletzungVerstauchungen und ZerrungenMeniskusrisse
Kreuzbänder sind die kurzen Bänder aus starkem, aber flexiblem Gewebe, die das Knie zusammenhalten und gleichzeitig Bewegungen des Kniegelenks ermöglichen. Manchmal kann eines oder mehrere der Kniebänder verletzt werden, zum Beispiel beim Sport oder infolge eines Autounfalls.
In diesem Artikel:
Videoauswahl für Sportverletzungen
Lesen Sie unten weiter
What are the knee ligaments?
There are four bones around the area of the knee joint: the thigh bone (femur), the main shin bone (tibia), the outer shin bone (fibula) and the kneecap (patella). The main movements of the knee joint are between the femur, the tibia and the patella.
Querschnittsdiagramm eines normalen Gelenks
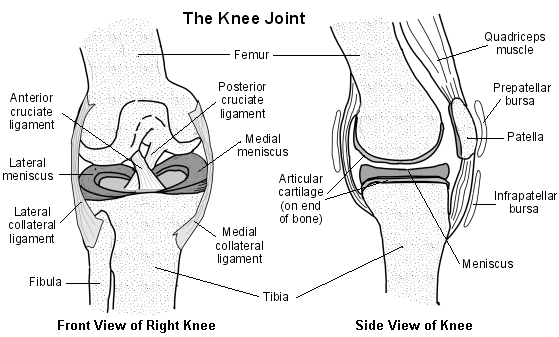
Tough connective tissue (articular cartilage) covers the ends of the tibia and femur and the back of the patella around the knee joint. The articular cartilage reduces friction between the bones of the knee joint and helps smooth movement between them.
Jedes Kniegelenk enthält ebenfalls einen inneren und äußeren Meniskus (einen medialen und lateralen Meniskus). Die Menisken (Plural von Meniskus) sind dicke, gummiartige Knorpelpolster. Sie sind C-förmig und werden zur Mitte des Gelenks hin dünner. Die meniskalen Knorpel liegen auf der, zusätzlich zur üblichen dünnen Schicht aus Gelenkknorpel, die die Oberseite des Schienbeins bedeckt. Die Menisken wirken wie Stoßdämpfer, um die Aufpralle des Oberschenkels auf den Unterschenkel abzufedern. Sie tragen auch dazu bei, die Bewegungen des Knies geschmeidig zu machen und das Knie stabil zu halten.
There are four ligaments around the knee joint. A ligament is a tough band of tissue that connects one bone to another bone around a joint. The knee joint ligaments help to stabilise and support the knee when it is moved into different positions.
Each ligament has a different job to do:
The medial collateral ligament (MCL)
This is one of the ligaments on the side of the knee joint. It runs between the femur and the tibia on the inner side of the knee. It helps to protect and stabilise the knee joint against any forces on the side of the leg. It helps to limit the amount that the knee moves from side to side.
The lateral collateral ligament (LCL)
This is the other main ligament on the other side of the knee joint. It runs between the femur and the fibula on the outer side of the knee. It helps to protect and stabilise the knee joint against any forces on the side of the leg. This ligament also helps to limit the amount the knee moves from side to side.
The anterior cruciate ligament (ACL)
This is one of the ligaments inside the knee joint. It runs diagonally connecting the front (anterior) of the tibia to the back (posterior) of the femur. This ligament helps to stabilise the knee joint by controlling backward and forward movements of the knee. It stops the tibia bone from moving forwards in front of the femur.
The posterior cruciate ligament (PCL)
This is the other ligament inside the knee joint. It also runs diagonally across the knee, connecting the back (posterior) of the tibia to the front (anterior) of the femur. The ACL and PCL cross each other inside the knee joint and some people call them the cross ligaments (cruciate means cross-shaped). The PCL helps to control the forward and backward movements of the knee.
The knee joint is surrounded by a protective joint capsule. This is lined by a special membrane called the synovial membrane. The synovial membrane produces synovial fluid which helps to lubricate and reduce friction within the knee joint. There are also muscles that help to support the knee joint. The main ones are the thigh muscles (quadriceps) and rear thigh muscles (hamstrings) in the legs.
What is a knee ligament injury?
Zurück zum InhaltThey may be stretched (sprained), or sometimes torn (ruptured). A ligament sprain happens when the fibres that make up the ligament are stretched and just a few fibres are torn. A rupture can be partial (more fibres are torn than in a sprain but the ligament is still intact) or complete (the ligament is torn through completely). The majority of knee ligament injuries are sprains and not tears and they tend to settle down quickly.
There are a number of different things that can cause injury to the ligaments in your knee:
You may have a direct blow to your knee or knock into something with your knee.
Your knee may be moved beyond its usual range of movement. For example, this can happen during a fall, if you land awkwardly during sport, or after a sudden twisting or movement.
Medial collateral ligament (MCL) injury
Injuries to the MCL can happen in almost any sport and can affect people of all age groups. They often happen when your leg is stretched out in front of you and the outer side of your leg receives a blow at the same time - for example, during a rugby or football tackle.
Lateral collateral ligament (LCL) injury
Injuries to the LCL are less common than injuries to the MCL. This is because your other leg usually protects against injury to the inner side of your knee. (It is usually a direct blow to the inner side of your knee that causes an LCL injury.) But, this ligament injury can sometimes happen if one leg is stretched out in front of you and doesn't have the other leg for protection - for example, during a rugby or football tackle.
Anterior cruciate ligament (ACL) injury
Anterior cruciate ligament (ACL) injuries most often occur during sports such as football, basketball, skiing and tennis. The injury happens if you land on your leg and then quickly pivot or twist your knee in the opposite direction while it is slightly bent.
Women are more likely than men to injure their ACL. Although it is not certain why this is, it is probably because, in general, the muscles around a woman's knee aren't as strong as those around a man's knee. About half of people with an ACL injury also have injury to their meniscus or another ligament in the same knee.
Posterior cruciate ligament (PCL) injury
Injuries to this ligament are not as common as ACL injuries. This is because the PCL is wider and stronger than the ACL. There are a number of ways that the PCL can become injured. For example, it may be injured during a car accident if the front of your bent knee hits the dashboard and your lower leg is forced backwards. It may also be injured from falling on to your bent knee. Your PCL can also be injured if your leg receives a blow from the front whilst it is stretched out in front of you with your foot on the ground - for example, during a game of football.
At first, some people with a PCL injury may not have much in the way of symptoms (see below). It may take a while for you to realise that there is a problem. For example, you may later notice pain that comes on when going up and down stairs or when starting a run; or, your knee may feel unstable when walking on uneven ground.
Lesen Sie unten weiter
How to identify a knee ligament injury
Zurück zum InhaltIf you have injured one or more of the ligaments in your knee, the symptoms are likely to be similar regardless of the ligament that is injured. The severity of the symptoms depends on the degree of the injury to the ligament. For example, a ligament that is completely torn may produce more in the way of symptoms than a ligament that is just sprained.
Symptoms can include:
You can hear a popping sound (or a popping or snapping feeling) at the time of injury - this can sometimes be heard (or felt) if a ligament is completely torn.
Swelling of your knee. When a ligament is injured, there may be some bleeding inside your knee joint from the damaged ligament. This can lead to knee swelling. The degree of swelling will depend on the severity of the injury. Minor ligament sprains may cause little in the way of swelling and the swelling may not appear for a few hours. However, completely torn ligaments may lead to a lot of knee swelling which comes on very quickly (within two hours) and is very painful.
Pain in your knee. Again, the degree of pain can depend on the severity of the knee injury.
Tenderness around your knee on touching. This may be mild tenderness over the actual ligament in minor sprains, or more generalised and severe tenderness if a ligament is torn.
Not being able to use or move your knee normally. In complete ligament tears, movement can be severely reduced; whereas, in more minor sprains, you may have a relatively good amount of knee movement.
A feeling that your knee is unstable or perhaps giving way if you try to stand on it. This may cause you to limp. Again, this depends on how severe the ligament injury is. You may be able to stand if you only have a minor sprain.
Bruising around your knee can sometimes appear, although not always. It may take some time for bruising to develop.
How is a knee ligament injury diagnosed?
Zurück zum InhaltIf you feel that you may have a knee ligament injury, you should see a doctor. Your doctor will usually start by asking you questions about the injury, what happened and where you are feeling any pain. They may then examine your knee to look for signs of pain and swelling of your knee joint. They may also move your leg into different positions to test your knee ligaments. From this examination, they may be able to get an idea of the possible injury that you have.
If your doctor is concerned that you may have a more serious knee ligament injury, they may refer you for further tests such as an ultrasound scan oder eine Magnetresonanztomographie (MRT). Such tests should be able to show up any tears or rupture of your ligaments. Sometimes, an X-ray of your knee may be suggested, if they suspect a fracture.
If you have a lot of swelling of your knee after your injury, doctors may sometimes suggest draining off some of the fluid that is causing the swelling in your knee. To do this, a needle can be used to pierce the skin around your knee and the fluid can be drained off into a syringe attached to the needle. Special precautions are taken to keep the area and the procedure sterile so as not to introduce infection into your knee joint.
Lesen Sie unten weiter
How to cure a knee ligament injury
Zurück zum InhaltSelf-help treatment
Denken Sie in den ersten 48-72 Stunden an:
PREIS - Protekt, Ruhen, WEis, CHöhe; ,E; und
Kein Schaden - kein Heilen, Aalkohol, RPREISM.
Paying the PRICE:
PSchützen Sie Ihr verletztes Knie vor weiteren Verletzungen.
Rest your affected knee for 48-72 hours following injury. Consider the use of crutches to keep the weight off your injured knee. However, many doctors say that you should actually not keep your injured knee immobile for too long. You can usually start some exercises to help keep your knee joint moving and mobile. Start these as soon as you can tolerate the exercises without them causing too much pain. You can ask your doctor to advise when you can start to move your knee joint and what exercises you should do.
WDie Anwendung sollte so bald wie möglich nach Ihrer Knieverletzung erfolgen – für 10-30 Minuten. Weniger als 10 Minuten hat kaum Wirkung. Mehr als 30 Minuten können die Haut schädigen. Kühlen Sie das Knie mit einem Eisbeutel, indem Sie Eiswürfel in einen Plastikbeutel oder ein Handtuch wickeln. (Direkter Kontakt mit der Haut sollte vermieden werden, da es zu Erfrierungen kommen kann.) Alternativ können Sie auch eine Tüte gefrorener Erbsen verwenden. Drücken Sie den Eisbeutel vorsichtig auf Ihr verletztes Knie. Die Kälte soll die Durchblutung des beschädigten Bandes verringern. Dies kann Schmerzen und Entzündungen lindern. Nach der ersten Anwendung empfehlen einige Ärzte, den Eisbeutel alle zwei Stunden für 15 Minuten während des Tages für die ersten 48-72 Stunden erneut anzuwenden. Während des Schlafs sollte kein Eis auf dem Knie verbleiben.
Compression with a bandage will limit swelling, and help to rest your knee joint. A tubular compression bandage can be used. Mild pressure which is not uncomfortable or too tight and which does not stop blood flow is ideal. A pharmacist will advise on the correct size. Remove before going to sleep. You may be advised to remove the bandage for good after 48 hours. This is because the bandage may limit movement of the joint which should normally be moving more freely after this time. However, bandages of the knee are sometimes kept on for longer to help keep swelling down and to keep the affected knee more comfortable. Ask your health professional what is best in your case.
EHeben soll Schwellungen begrenzen und verringern. Zum Beispiel halten Sie Ihren Fuß auf der betroffenen Seite beim Sitzen auf einem Stuhl mit einem Kissen unter dem Knie. Es ist möglicherweise einfacher, sich auf ein Sofa zu legen und den Fuß auf einige Kissen zu legen. Wenn Sie im Bett sind, legen Sie den Fuß auf ein Kissen. Das Ziel ist, dass Ihr betroffenes Knie über dem Herzniveau liegen sollte.
R is sometimes added to this list to make PRICER. R stands for Rehabilitation which is the most important part of the treatment for knee ligament injuries - to get you and your knee back to normal. You may need to see a physiotherapist or sports therapist for advice about exercises to do to strengthen and stretch the muscles around your knee if your symptoms persist.
Hinweis: despite the common guidance of putting an ice-pack on injuries, there is some evidence from animal studies that it can delay healing and some researchers in the field suggest the evidence for putting ice on an injury is not very strong.
Vermeiden Sie SCHADEN für 72 Stunden nach der Verletzung. Das heißt, vermeiden Sie:
Hessen – zum Beispiel heiße Bäder, Saunen, Wärmepackungen. Wärme hat die entgegengesetzte Wirkung zu Eis auf den Blutfluss. Das heißt, sie fördert die Durchblutung. Daher sollte Wärme vermieden werden, wenn sich eine Entzündung entwickelt. Nach etwa 72 Stunden ist jedoch wahrscheinlich keine weitere Entzündung mehr zu erwarten, und Wärme kann dann beruhigend wirken.
AAlkoholische Getränke, die die Blutung und Schwellung verstärken und die Heilung beeinträchtigen können.
RJoggen oder andere Sportarten, die weiteren Schaden verursachen könnten.
MMassage, die die Blutung und Schwellung verstärken kann. Nach etwa 72 Stunden kann jedoch eine sanfte Massage, ähnlich wie bei Wärme, beruhigend wirken.
Medikation
Paracetamol und Codein: Paracetamol ist hilfreich zur Schmerzlinderung. Es ist am besten, Paracetamol regelmäßig über einige Tage einzunehmen, anstatt nur gelegentlich. Eine Erwachsenendosis sind zwei 500 mg Tabletten, viermal täglich. Bei stärkeren Schmerzen kann Ihnen ein Arzt ein anderes Medikament verschreiben Codein, das stärker ist, aber bei manchen Menschen schläfrig und verstopft machen kann.
Entzündungshemmende Schmerzmittel: these medicines are also called Nichtsteroidale entzündungshemmende Medikamente (NSAIDs). Sie lindern Schmerzen und können auch Entzündungen und Schwellungen begrenzen. Es gibt viele Arten und Marken. Sie können einige kaufen (zum Beispiel, Aspirin und Ibuprofen) at pharmacies, without a prescription. You need a prescription for others. Side-effects sometimes occur with anti-inflammatory painkillers. Stomach pain, and bleeding from the stomach, are the most serious. Some people with Asthma, Bluthochdruck, Nierenversagen, schlecht Verdauungsstörungen und heart failure may not be able to take anti-inflammatory painkillers. So, check with your doctor or pharmacist before taking them in order to make sure they are suitable for you.
Aber beachten Sie: National Institute for Health and Care Excellence (NICE) Clinical Knowledge Summaries (CKS), a well-known source of guidance for doctors in the UK, do not recommend that anti-inflammatory painkillers be used in the first 48 hours after the injury. This is because of concerns that they may delay healing. The logic is that some inflammation is a necessary part of the healing process. So, it may be that decreasing inflammation too much by taking these medicines may impair the healing process. This is a supposed (theoretical) concern, as no trials have proved this point. Further research is needed to clarify the use of these medicines following an injury.
Also, if you are having surgery to repair a torn ACL (see below), it is thought that, theoretically, NSAIDs may not be a good idea to take for a long period of time after the surgery because they may have an effect on the success of the surgery.Äußerliche (topische) entzündungshemmende Schmerzmittel: again, there are various types and brands of äußerlich anwendbaren entzündungshemmenden Schmerzmitteln. You can buy some, without a prescription, at pharmacies . You need a prescription for the others. There is debate as to how effective rub-on anti-inflammatory painkillers are compared with tablets. Some studies suggest that they may be as good as tablets for treating sprains. Some studies suggest they may not be as good. However, the amount of the medication that gets into the bloodstream is much less than with tablets, and there is less risk of side-effects.
Physiotherapie
Physiotherapy may be helpful after some knee ligament injuries. A physiotherapist or sports therapist may be able to help you to improve the range of movement in your injured knee. Exercises will also be suggested for you to do regularly at home to help strengthen the muscles that support your knee joint. If you are considering surgery to repair a torn knee ligament, you may be advised to see a physiotherapist before the operation.
Knee braces
Depending on the knee ligament injury that you have, your health professional may advise you to wear a special brace to support your knee while the damaged ligament heals. Knee braces usually have a hinge mechanism that allows some bending and extending movement of your knee joint. The mechanism does not allow movement of your knee from side to side. However, a knee brace may not be advisable for all knee ligament injuries. You may like to discuss the use of a knee brace with your doctor.
Operation
Sometimes surgery may be suggested after a knee ligament injury. This is more likely if:
You are someone who does a lot of sport or you are a very active person and you have injured your ACL.
You have injured more than one knee ligament, or you have injured a knee ligament and have also injured another part of your knee.
You have ruptured your LCL.
Physiotherapy and rehabilitation have not helped.
Surgery is most commonly suggested to repair ACL injuries. However, it is fair to say that the best way to treat a torn ACL is still debated. Physiotherapy and other measures may be all that is needed by some and may prevent the need for an operation. The decision about whether or not to use surgery depends on:
How effective physiotherapy has been in relieving your symptoms.
The activities and sports that you do.
How active your lifestyle is in general.
Your underlying health.
Any other knee injuries that you may also have.
You may want to discuss the pros and cons of surgery with your doctor.
If surgery is carried out to repair a torn ACL, your doctor will usually advise that you wait some weeks after your initial injury. This is so that:
Any swelling has had a chance to go down.
Physiotherapy and rehabilitation have had a chance to work:
You have got more movement back in your knee.
You have built up the strength in the muscles of your thighs that help to support your knee joint.
The ACL cannot simply be stitched back together. Instead, surgery to reconstruct, or rebuild, the ACL is usually carried out. Most often, part of a tendon, or tendons, from somewhere else in your body is used to reconstruct your ACL. For example, the following may be used:
Part of the tendon at the bottom of your kneecap (your patellar tendon).
Part of the tendon that attaches your kneecap to the quadriceps muscle at the front of your thigh (your quadriceps tendon).
Part of the tendons that run from the back of your knee up the back of your thigh (your hamstring tendons).
Sometimes, tendons from someone else (a donor) may be used to repair your ACL.
The tendon is fixed in place inside your knee joint, using staples or screws. Once fixed in place, over time, a new ligament should grow over the tendon that has been used. Keyhole surgery is usually used to reconstruct your ACL.
There is some debate as to the best way to treat PCL injury - with surgery, or without surgery. You may like to discuss this with your doctor. If surgery is carried out, as with surgery for ACL injury, the damaged ligament is replaced using a tendon, or tendons, from elsewhere in your body, or using a donor tendon.
Surgery is not often needed for MCL injuries.
How to strengthen knee ligaments after injury
One of the best ways to strengthen knee ligaments after injury is simply to keep them moving and keep them loose. Although there is a great deal of information on the internet about the best stretches and strengthening exercises, it is very important to do the correct stretches and strengthening exercises for your particular injury, and the supervision of a physiotherapist can be very important for recovery.
How long does a knee ligament injury take to heal?
Zurück zum InhaltThis will depend on which knee ligament you have injured and also how severe your injury is. Also, if you have injured more than one ligament in your knee, recovery may take longer.
If you have surgery to repair your ACL, it usually takes around six months before your knee has recovered enough for you to return to your previous sporting activities. However, in some people, it may be longer. In general, surgery to reconstruct an ACL has good results in up to 8 out of 10 people in the short term but the risk of a second ACL injury is high, especially in young athletes. In the longer term, many people who have had an ACL tear develop Osteoarthritis in their knee, whether or not they have had their ACL reconstructed.
If your PCL has been treated using surgery, it can take between 9 and 12 months before complete recovery.
After a stretch injury (sprain) or partial tear to the MCL, the ligament has completely healed in most people after three months. If there is a complete tear, recovery may take a little longer but most people are back to their usual activities after 6-9 months.
Hinweis: you should ask advice from your medical professional about when it is safe for you to start exercise or sport again after a knee ligament injury. It is important that you do not start exercising again until your knee is pain-free and completely stable. If you start exercising too early, you may cause further injury to your knee.
Can knee ligament injuries be prevented?
Zurück zum InhaltKnee ligament injuries can be unpredictable and can affect anyone, including fit people who do a lot of sport. Exercising regularly is recommended. Building up the strength in the leg and hip muscles that help to support your knee joint (particularly your hamstring and quadriceps muscles) may help to reduce your chance of knee ligament injury. If you are not used to exercising regularly, you should start gently and gradually build up the frequency and intensity of your exercise. See the separate leaflet called Physical Activity for Health for more details.
During an exercise session, or if you are playing sport, make sure that you warm up at the start of your training. Warming up means 5-10 minutes of balance exercises and gradually increasing your activity. This increases the flow of blood to your muscles and helps to loosen up your joint movements. Warming up may also help to prevent injury.
Some people wear a knee brace when they are exercising or doing sporting activities if they have previously had a knee ligament injury, or even just to prevent a knee injury in the first place. Some studies have shown that wearing a brace may help to reduce the chance of another injury. Other studies have not shown this to be the case. One particular study looked at people with previous injury to their ACL. The study found that those who wore a knee brace whilst skiing were less likely to have a further knee injury than those who did not wear a knee brace. In general, more research is needed to look at the use of knee braces for preventing knee injury.
Patientenempfehlungen für Sportverletzungen

Knochen, Gelenke und Muskeln
Knöchelverletzung
Das Sprunggelenk ist ein kompliziertes Gelenk und wird häufig verletzt. Fast die Hälfte der Verletzungen resultiert aus dem Sport oder dem Training. Eine Verstauchung des Sprunggelenks ist die häufigste Sportverletzung.
von Dr. Hayley Willacy, FRCGP

Knochen, Gelenke und Muskeln
Verstauchungen und Zerrungen
Verstauchung ist eine Verletzung des Bandes (Ligament), das zwei oder mehr Knochen mit einem Gelenk verbindet. Eine Verstauchung wird in der Regel verursacht, wenn das Gelenk plötzlich außerhalb seines üblichen Bewegungsbereichs gezwungen wird. Eine schwere Verstauchung kann aussehen und sich anfühlen wie ein Bruch (Fraktur), und es kann für medizinisches Fachpersonal schwierig sein, den Unterschied zwischen beiden zu erkennen. Eine Zerrung bezieht sich auf eine Überdehnung und Rissbildung in Muskeln oder Sehnen. Nach einer Verstauchung oder Zerrung lautet der übliche Rat, die PRICE-Methode (Protection, Rest, Ice, Compression, and Elevation) anzuwenden und HARM (Heat, Alcohol, Running, and Massage) in den ersten 48-72 Stunden nach der Verletzung zu vermeiden. Die meisten Verstauchungen und Zerrungen heilen innerhalb weniger Wochen. Hinweis: Dieses Merkblatt gibt keine Hinweise dazu, wie man die Art der Verletzung unterscheiden kann. Zum Beispiel ist es manchmal schwierig zu erkennen, ob man einen Knochenbruch oder eine andere ernsthaftere Verletzung hat. Daher sollten Sie einen Arzt oder eine Krankenschwester aufsuchen, wenn Sie vermuten, dass Sie einen Bruch oder eine andere ernsthaftere Verletzung haben. Dieses Merkblatt geht davon aus, dass Sie wissen, dass Sie eine Verstauchung oder Zerrung haben (zum Beispiel, weil Ihnen dies ein Arzt oder eine Krankenschwester gesagt hat) und nichts Schwerwiegenderes.
von Dr. Doug McKechnie, MRCGP
Weiterführende Lektüre und Referenzen
- Sports Injury Rehabilitation Exercises; Sportsinjuryclinic.net
- Andrews K, Lu A, Mckean L, et al; Review: Medial collateral ligament injuries. J Orthop. 2017 Aug 15;14(4):550-554. doi: 10.1016/j.jor.2017.07.017. eCollection 2017 Dec.
- Ng JWG, Myint Y, Ali FM; Management of multiligament knee injuries. EFORT Open Rev. 2020 Mar 2;5(3):145-155. doi: 10.1302/2058-5241.5.190012. eCollection 2020 Mar.
- Filbay SR, Grindem H; Evidence-based recommendations for the management of anterior cruciate ligament (ACL) rupture. Best Pract Res Clin Rheumatol. 2019 Feb;33(1):33-47. doi: 10.1016/j.berh.2019.01.018. Epub 2019 Feb 21.
- Kew ME, Cavanaugh JT, Elnemer WG, et al; Return to Play after Posterior Cruciate Ligament Injuries. Curr Rev Musculoskelet Med. 2022 Dec;15(6):606-615. doi: 10.1007/s12178-022-09794-z. Epub 2022 Nov 30.
Lesen Sie unten weiter
Artikelverlauf
Die Informationen auf dieser Seite wurden von qualifizierten Klinikern verfasst und begutachtet.
Nächste Überprüfung fällig: 9. Feb 2028
10. Feb 2023 | Neueste Version
25 Nov 2010 | Ursprünglich veröffentlicht
Verfasst von:
Dr Michelle Wright, MRCGP

Fragen, teilen, verbinden.
Durchsuchen Sie Diskussionen, stellen Sie Fragen und teilen Sie Erfahrungen zu Hunderten von Gesundheitsthemen.

Fühlen Sie sich unwohl?
Bewerten Sie Ihre Symptome online kostenlos
Abonnieren Sie den Patienten-Newsletter
Ihre wöchentliche Dosis klarer, vertrauenswürdiger Gesundheitsberatung - geschrieben, um Ihnen zu helfen, sich informiert, selbstbewusst und in Kontrolle zu fühlen.
Mit dem Abonnieren akzeptieren Sie unsere Datenschutzrichtlinie. Sie können sich jederzeit abmelden. Wir verkaufen Ihre Daten niemals.